Mapping Cellular Gap Junctions to Understand Disease
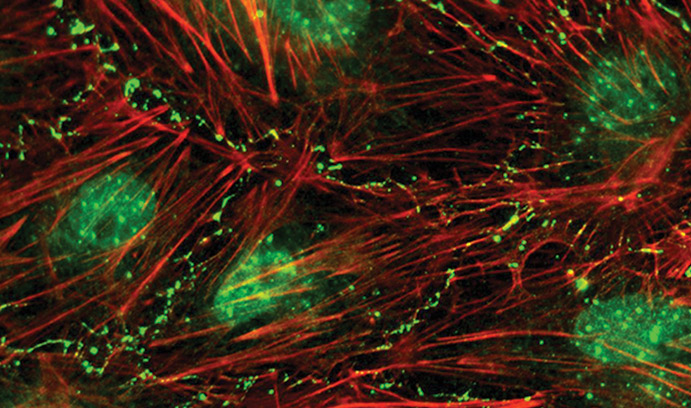
Matthias Falk is mapping the life cycle of cellular gap junctions to unlock the mystery of mutations that cause disease. (Image courtesy of Matthias Falk)
Cellular Communication
Few have a better understanding of the life cycle of a gap junction than Matthias Falk and his team. Falk has spent the last 14 years studying the internal machinery of the final stage of the life of gap junctions—the channels through which cell-to-cell communication occurs.
Ultimately, his goal is to gain a deep understanding of how gap junctions function, to better understand what happens when they malfunction.
"We need to understand what's normal before we can know what is not normal," says Falk, professor of biological sciences.
Gap junctions are special. They are the only known cellular structures that allow a direct transfer of signaling molecules from one cell to another by forming hydrophilic (water filled) channels that bridge the plasma membranes of neighboring cells. One cell provides half of the channel, a neighboring cell provides the other half. The halves connect to form one channel that allows the two cells to send signals directly into each other's cytoplasm.
Proteins called connexins form the building blocks of gap junctions. A number of diseases are associated with connexin mutations, including diseases of the heart, cataracts, hearing loss, neuropathies, skin and bone disorders, and cancer. However, there is little understanding of how these gap junctions are assembled, maintained and then degraded—much less how these processes could go awry.
"My lab has focused on the degradation phase of the gap junction life cycle—after the cell has built and then maintained the structure—because impaired removal of the channels is linked to disease," says Falk.
Falk and his team are able to observe and characterize a gap junction's life cycle in living cells through immunofluorescent microscopy using a process called transfection. They fuse the DNA of a green fluorescent protein to tag the connexin protein of interest and then push it through a cell membrane—in much the same way a virus infects a healthy cell. When lit, the tag enables them to observe the proteins.
"We can follow, in real-time, the degradation process, watching how the old structure is internalized into the cell, becomes a vesicle within the cell's cytoplasm and moves away from the plasma membrane," says Falk. "This is how we have been able to obtain an understanding of the complex internal machinery driving the gap junction internalization process on the molecular level."
Characterizing these complex cellular processes is key to developing treatments for disease.
"Before a drug can address a mutation in the gap junction that is causing something to go wrong, we need to find out what it looks like when it goes right," adds Falk.
Falk's work could be classified under what the National Institutes of Health have dubbed Bench-to-Bedside science. This refers to research that translates basic scientific findings into therapeutic interventions for patients and increases understanding of important disease processes.
Through their study of gap junctions, Falk and his team hope to exemplify the bench that may one day make treatment a reality at a patient's bedside.
This story appears as "Cellular Communication" in the 2017 Lehigh Research Review.
Posted on:




